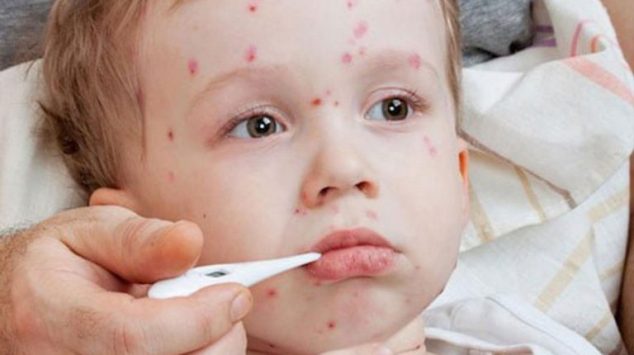
What is a need of Pediatrics dermatology? We understand your concern. A Pediatric dermatologist is a certified specialist for the treatment of wide ranges of conditions, with the most specific being bacterial, fungal and viral infections; hemangiomas and atopic dermatitis. As a best Pediatric Dermatology related Specialists in Delhi (West Delhi), we are dedicated to provide the people with best maintenance of skin’s health using non-invasive therapy. Any damage caused to your skin due to exposure to sun/pollution, weather change, atmospheric allergens, and multitude of remedies can be cured effectively taking advice from dermatologist in Delhi.
Here we are talking in detail about the skin disease found in children, how to cure & how to take care of the issues.
Table of Contents
Paediatric dermatology deals with the dermatological or skin problems that children face. A paediatric dermatologist diagnoses and treats the skin, hair and scalp conditions of children and infants. He/she prescribes treatment and suggests medical or surgical procedures for skin conditions such as warts and other lesions of the skin.
Children having dermatological conditions can take advice and benefit from the experience and expertise of recognized physicians. Dr. Rohit Batra’s Dermaworld Skin Institute is one of the best skin clinics in Delhi offering consultancy on paediatrics dermatology.
Children who have usual dermatological conditions can take advantage from the proficiency of specialized physicians. Although, adults may develop some complaints but they differ considerably when dealing with a skin problem in childhood. Dermatologists in Delhi offer treatments with the help of state-of-the-art technologies.
The treatment suits the skin of a child or an adolescent. The dosage is dependent on the weight of the child. Thus, it is important that skin diseases in children are treated by highly experienced dermatologists who have an expertise in this field.
Paediatric dermatology mainly concentrates on the treatment of children from birth to their teenage years, as it is the most common time for skin disorders. During this age, common diseases like ringworm, chickenpox, acne, eczema or birthmarks can occur.
Infants and children are particularly susceptible to eczema. The most commonly noticed paediatric skin disorders are vascular (red) birthmarks, moles or warts, skin rashes, poison ivy, ringworm, hives, and cradle cap. Acne can also appear in adolescence and cause scarring affecting the self-esteem of children. Dr. Rohit Batra is one of the best dermatologists in Delhi offering quality skin treatments.
We have excellent medical facilities and are engaged in offering diagnosis and treatment for various paediatric skin disorders such as eczema, acne, contact dermatitis, psoriasis, congenital skin allergies, and removal of birthmarks, warts and vascular (red) moles. Young children are prone to become impatient as they are not able to answer the medical questions properly or communicate, thus need special care. Our medical team has rich experience in dealing with children and take every possible step to make them feel better. We provide a range of both surgical and non-invasive procedures to treat all kinds of skin diseases. Skin specialists in Delhi are trained from top most institutes and make certain to treat all skin conditions aesthetically.
Skin is the largest organ of the body and serves as multiple functions ranging from acting as an epithelial barrier to maintaining body temperature. Skin diseases are often occurring diseases in pediatric age group and amounts to maximum pediatric visits in India. This is more so because a child’s skin is more delicate as compared to adults and hence are more prone to any infections.
Moreover, on a child’s body, finding a bump, rash, red mark, or zit is far more common rather than not finding one. Most of these are not serious; but, few of them may be associated with concern and should be dealt promptly in which cases visiting a pediatric dermatologist can save time.
In India, skin diseases primarily manifest as infections and infestations, which are secondary to infections in the body but the good thing is that dermatologists can promptly diagnose and treat skin diseases. However, general awareness among parents can help in early diagnosis and timely management of these diseases. The best way of getting skin diseases treated is getting it treated in right time, to avoid spread to other areas within the patient’s body.
Impetigo is a communicable, superficial infection of the skin more common in kids (specifically 2- to 5-year-olds) than in adults which are caused by Streptococcus (strep) and Staphylococcus (staph) bacteria. The development of Impetigo is most possibly to happen in warm and humid climate and is spread by close contact (like between family members). The disease being communicable spreads in children even from sharing toys, towels or toiletries.
There are two forms of impetigo i.e. Nonbullous and Bullous impetigo. The Nonbullous impetigo is typically presented by small red papules similar to insect bites which quickly evolve into tiny blisters and then to pustules that eventually scab over with a honey-colored crust. While the Bullous impetigo looks like fragile blisters filled with clear yellow-colored fluid.
Clinical diagnosis of impetigo disease is easy by assessing the affected area & if the infection keeps recurring. Further tests may be ordered to find if disease occurred due to another skin condition, such as scabies. Parent, patient or caregiver is investigated about any recent insect bites, cuts, or to the affected area, to find out the exact cause of the condition.
During diagnosis, the crusted area will be gently wiped with a swab to check which germ is causing impetigo and which antibiotic or treatment type is most likely to work.
Without treatment, impetigo can become infected, and complications may result. The medical treatment for impetigo depends on the type and severity of symptoms, but can be successfully treated. Treatment for impetigo aims at removing crusts, speed up healing, improve skin’s appearance, and prevent spread of infection and complications.
Prescription-strength antibiotic and topical ointment guided by laboratory results help heal impetigo completely and quickly. For mild impetigo infection, a gentle skin cleansing regimen can be recommended.
There may be a revolving concern about will impetigo leave scars? There are rare chances of marks left as the blisters and crusts of impetigo are superficial and usually do not leave scars. Affected skin appears red for a while after the crusts vanishes, but this redness fades in several days.
Impetigo can possible be prevented by following routine hand-washing. If the signs of infection show up, infected area should be covered with bandage during this time.
A dermatologist, primary-care doctor or pediatrician, holistically as well as routinely can manage treatment of impetigo.
A rarely called Ecthyma is the medical term used for a rash similar to impetigo or an ulcerative form of impetigo, but the infection perforates in the skin more deeply. Development of Ecthyma is likely to take place in a moist atmosphere, ill hygiene, or long-standing nasopharyngeal carriage of staphylococci.
Small, superficial, overripe, punched-out ulcers with thick, brown-black crusts typically characterize ecthyma, that cause mild pain or discomfort in the affected area. Scratching may cause spread infection, in the surrounding as well as non-surrounding skin.
Diagnosis of Ecthyma is conducted by characteristic appearance. Cultures of lesions are manifest under instances of patient not responding to empiric therapy. An effective course of treatment for Ecthyma includes Topical retapamulin, mupirocin, fusidic acid or sometimes oral antibiotics.
With timely and appropriate treatment follows prompt recovery. Delay in medical assistance can cause furunculosis, lymphangitis, cellulitis, and hypopigmentation or hyperpigmentation with or without scarring.
As a general rule of care, make sure to wash the affected area gently with soap and water couple of times a day to cast aside any crusts.
Bacteria on the skin can contribute towards infection of one or more hair follicles. A hair follicle is a part of skin or connective tissue that regulates hair growth. There are 3 different kinds of infections that are triggered with ulceration in follicles:
One disturbing element about these skin infections is that these can appear anywhere on the skin where there is hair. The main cause of trigger is accumulation of excessive sweat and rubbing. It happens most often at the back of the neck, armpits, waist, groin, buttocks or face.
Bacteria called Staphylococcus aureus (staph) is the most common cause of folliculitis, furuncles, and carbuncles in a child, while anyone can be at a risk to develop these contagion. Children may be more at risk if he or she:
A single or group of skin lesions that are red, swollen, warm, leaky (pus) and painful indicate these infection. Affected person may also feel fever and chills with low blood pressure and fast heart beat.
A physical examination of the skin is performed to confirm folliculitis, furuncles, and carbuncles. A sample of the pus from the infection can be sent to a lab to see what type of bacteria caused the infection and accordingly help the doctor decide the best treatment.
Treatment for folliculitis, furuncles, and carbuncles treated will depend upon the symptoms, age, and health conditions and of course how severe the disease is.
Mild Folliculitis and furuncles may ride off with no treatment. Compresses may help calm off symptoms and speed healing. Moderate to severe Folliculitis, furuncles and carbuncles are often treated by incision and draining, where a healthcare provider cuts into the lesion and drains the fluid (pus) out. A medication by mouth (oral) or in a vein (IV) may also be given.
To help prevent these infections, make sure to clean and protect any skin injuries, use clean razors, nails cut short and stay away from others with these infections and you are rectified. But do not leave the conditions untreated as they may lead to possible complications of returning of infection, spreading to other parts of the body and scarring.
Peri Anal Streptococcal is an infection of the anus and rectum caused by the germ called Streptococcus. There are alternatives names used for the disease such as Streptococcal proctitis; Perianal streptococcal dermatitis, Proctitis – streptococcal. The problem generally occurs in children, commonly during or after strep throat, nasopharyngitis, or impetigo.
Children may end up callusing the skin around the anus while cleaning the area using a harsh toilet paper, by scratching with hands that have bacteria or not properly washed the defecate.
If there is itching, bleeding or pain in the bowel movement or sever redness around the anus, it may indicate the problem.
The health care provider may ask for some tests or exams including:
A course of antibiotic treatment, generally for 10 days is directed, depending on how well and effectively the patient is responding. Children generally show quick recovery with antibiotic treatment. So, make sure to put across your health care provider if your child does not get better soon on antibiotics.
Topical medicine can be used in conjunction with antibiotics to ease itch and pain in the area, but should not be the standalone treatment. A common topical medicine used for this condition is Mupirocin.
Complications out of this problem can be really cruel with anal scarring, abscess or fistula, anal discharge, bleeding, or bloodstream infections and severe skin and soft tissue infection.
To prevent the condition from coming back and further complications, ensure to take timely treatment in a prescribed form.
Diaper dermatitis occurs due to prolonged contact with skin and face and many cases get infected secondarily with bacteria and candida albicans. These dermatitis conditions are somehow in one or the other way related to diapers that the baby wears and there are three main types of diaper dermatitis i.e. chafing dermatitis, irritant contact dermatitis and candida diaper dermatitis.
Young babies often get heat rash. Blocked sweat glands cause heat rash, which results in a red pimply eruption on the head and neck. It’s important to dress your infant appropriately (not too hot and not too cold) to prevent the eruption. Generally, heat rash resolves on its own.
Epidermis and its appendages are not well differentiated at birth, particularly in cases of preterm infants which often leads to sweat retention phenomenon which are vesicular eruptions followed by maceration and obstruction of eccrine sweat glands as the ducts of the sweat glands are relatively immature.
They are more common in first few weeks. They are mainly of two types, milia crystalline (sudamina) are clear fluid filled pin point vesicles which are superficial and milia rubra (pricklyheat)is seen as small erythematous, macules, papules, vesicles or papulovesicular. Therapy is directed towards minimizing excess heat and humidity. Light weighted cotton clothes and cool baths are advocated and usually there is no need of any treatment or medication.
Herpes zoster, or shingles, is caused due to reactivation of the varicella-zoster virus (chickenpox). The virus causes a painful rash of small blisters on a part of skin anywhere on the body. On some occasions, there can be pain for a prolonged period of time even after the rash subsides.
Once a person has had chickenpox, the virus resides dormant in the nerves. If the virus gets reactivated later in life, it causes shingles. Herpes zoster is relatively more common in people with compromised immune systems or over the age of 50. It is very rare in children, and even then, the symptoms are mild as compared to adult.
However, Children who have depressed immune systems can experience the same, or severe, symptoms as adults.
Herpes zoster often occurs on the trunk and buttocks, but can also appear on the arms, legs, or face. The symptoms vary as per individual and each child may experience different symptoms. The commonly presenting symptoms may include skin hypersensitivity in the areas affected by herpes zoster.
Mild rash, that appears after five days and initially looks like small, red spots turn into blisters, which usually subsides over a week. The lesions are always unilateral in presentation owing to the involvement of specific nerve.
Diagnosis of herpes zoster is usually clinically obtained by a recent medical history of the child and performing a physical examination. Diagnosis may also include skin scrapings (gently scraping of the blisters to determine the virus type) and Blood tests.
Specific treatment plan for herpes zoster has to be determined by a physician based on the child’s age, systemic health, medical history, severity and extent of the condition and the child’s tolerance and compliance for specific drug regime and procedures as well as the expected outcome for the course of the disease. The Child or parent’s preference can also be taken into account while formulating a treatment plan.
Medication can only help in alleviating some of the pain, but the viral condition has to undergo its course. Immediate treatment with antiviral drugs may help to lessen some of the symptoms. Drug dosage and type of medication will be determined by a physician based on the age of the child or body surface area and the severity of the disease.
Measles is caused by a single-stranded ribonucleic acid (RNA) virus of the family Paramyxoviridae. Infection begins in the nasopharyngeal epithelium and less commonly through the conjunctivae. Transmission of measles is primarily via respiratory droplets and less commonly by small particle aerosols. The incubation period is around 10 to 14 days. The virus enters the lymph nodes and lymphatics and multiplies within the reticuloendothelial system which results in subsequent viremia.
The virus is then disseminates to multiple lymphoid tissues and other organs, including the skin, liver, and gastrointestinal tract. Immunity to measles is mediated by cell-mediated, humoral, and mucosal responses. Measles antibodies are responsible for protection from future infection or re-infection in the course of life. The classical features of measles are fever and cough, coryza, and conjunctivitis.
The pathognomonic spots called as, Koplik spots, that are usually prodromal in nature and presents with punctuate, gray-white to erythematous papules spread on the buccal mucosa in the posterior molar region. It begins on the face especially the forehead, hairline, and behind the ears, and spreads downward onto the trunk and extremities.
warts are caused by viruses and are small sized skin bumps. They are caused by human papillomavirus. Warts can spread both from person to person and to other parts of the body of the same individual. Most common site of occurrence of warts is hand, but they can occur anywhere. Many resolve on their own, but there are over-the-counter medications available to speed up resolution and treatment may take weeks.
Contact dermatitis appears as a group of small red pimples or bumps on a skin surface exposed to some sort of allergen. These allergens can be due to specific foods, lotions, chemicals, or plants, such as poison ivy. The rash starts within one to two days of exposure, depending upon the sensitivity and can last for as long as the exposure with the allergen continues or until it heals, which usually takes one to two weeks. Topical antihistamines or steroids may decrease the symptoms.
Hives occur as a result of a dermal allergic reaction. They appear as small red itchy bumps or welts, which may be painful depending on the severity of the lesion. Exposure to an allergen, such as a food or medicine, may cause hives. Some common allergies include nuts, eggs, and shellfish, but certain viruses can also cause hives.
However, hives alone are not dangerous, if your child develops breathing troubles, including cough and wheezing along with the hives, it can be an emergency situation requiring immediate medical attention and management. The standard treatment for hives is antihistaminics.
Coxsackievirus occurs in three forms and causes three different types of diseases. One of the variants cause hand, foot, and mouth disease. It is an extremely common childhood infection, especially during the summer season and early rainy fall. It usually starts with fever and then develops into a non-itchy rash involving the body, typically involving the hands and feet; it also causes mouth sores.
The mouth sores are painful and can interfere and restrict eating and drinking in some cases leading to further weakness and state of disease. It is extremely contagious, and like most viral infections, it spreads through direct contact, often by coughing and sneezing. Hand, foot, and mouth disease resolves on its own within weeks.
Streptococcal infection causes scarlet fever, a very commonly occurring illness that begins with a sore throat, fever, malaise and other nonspecific complaints. The rash, which starts after the other symptoms, feels like sandpaper and may or may not be itchy.
Pastia lines are characteristic feature seen on skin folds. Its manifestations are also seen on tongue known as strawberry and raspberry tongue. Scarlet fever is highly contagious, and although it generally resolves on its own. It is necessary to treat the underlying strep tococcal systemic infection with antibiotics.
SSSS is a term which encompasses a blistering skin disease caused by the epidermolytic (or exfoliative) toxin (ET)-producing S. aureus. The pathogenesis of SSSS is due to the production of ETs, of which there are two different serotypes affecting humans, ETA and ETB. SSSS usually begins with localized infection of the conjunctivae, nares, perioral region, perineum, or umbilicus.
Removal of perioral crusts leaves behind radial fissures around the corners of mouth, resulting in the characteristic facial appearance of SSSS. Other infections that can serve as the initial nidus for SSSS include pneumonia, infective endocarditis, septic arthritis, or pyomyositis. Fever, malaise, irritability, and poor feeding subsequently progress, lead to generalized eruption.
The rash is characterized by erythema that enlarges to large, superficial fragile blisters that rupture easily and result in denuded, desquamating, erythematous, and tender skin. The eruption is most marked in flexural creases but can also sometimes involve the entire surface area of skin. The Nikolsky’s sign (progression of the blister upon gentle pressure on the edge of the bulla) is positive. The most reliable distinguishing feature of TEN is mucosal involvement that involves the corner of the mouth, conjunctivae, trachea, and genital mucosa, which is not seen in SSSS.
It is worth to be noted that the majority of blisters in SSSS are sterile, as they are caused by the hematogenous dissemination of the bacterial toxin and not by the spread of bacteria itself. Treatment of SSSS is directed at the eradication of toxin-producing staphylococci and thus terminating toxin production and its dissemination.
Besides these infections and their manifestations, the other commonly occurring dermal infestations are Head lice. Head lice usually affect children between 3 and 12 years by direct head to head contact. Scalp itching is the most common as well as primary symptom and may be accompanied with redness, papules, excoriated lesions and secondary bacterial infections.
The secondary infections can cause Occipital and cervical lymphadenopathy occasionally. Diagnosis is confirmed by the presence of nits or lice in the scalp and hair. Nits are grey white, 1 mm sized, ovoid eggs that are firmly attached to the hair shaft.
The treatment of choice is 1 % permethrin cream that should be applied to mildly damp hair, followed by rinse after 10 min. A repeat application is usually recommended after 1 or 2 weeks. In children older than 5-year oral Ivermectin can be used.
Tinea Capitis is the most common dermatophyte infection and is usually seen in pre-pubertal girls (3–7 y). T. Capitis (grey patch) presents with single or multiple patches of alopecia along with inflammatory signs of papules, pustules, crusting and scaling. Hair is easily pluckable in these patches.
Tinea versicolor is a commonly occurring skin condition that occurs in older children and young adolescents and is caused by Malassezia furfur. It is frequently seen in tropical countries due to high humidity. It presents as numerous hypopigmented scaly macules on the upper part of chest, back and proximal upper extremities.
Potassium hydroxide test from the skin scraping is used to demonstrates short non-branching hyphae and yeast cells which aids in diagnosis. The treatment options readily available, includes topical selenium sulfide 2.5% lotion, imidazoles, ciclopirox olamine and sulfur preparations. Oral ketoconazole or fluconazole 400 mg can also be used. Management consists of reassuring and educating the parents regarding the benign nature of the lesion.
Atopic Dermatitis or eczema is a chronic and relapsing inflammatory skin disease. The hallmark of atopic dermatitis is Xerosis (dry skin) and pruritus. It usually starts in the initial first few weeks or months of neonatal life. The clinical phase of atopic dermatitis is divided into 3 groups, based on the onset and distribution of the lesions; infantile; childhood and adult phases.
In the infantile phase, the dermatitis usually starts on the face and then may spread to trunk. The affected infants are irritableor are often seen scratching the lesion due to intense pruritus.
It is characterized by symmetrical erythematous papules, vesicles, edema, exudation/oozing and crusting. The extensor aspect of the extremities of the limbs, are affected around 8 months of age the time around when they start crawling. Infantile atopic dermatitis usually spares the groin and buttocks. In the childhood phase, the lesions become chronic and lichenified with a predilection for the flexural areas (cubital and popliteal fossae).
In the face, peri-oral and per-orbital areas may also show chronic dermatitis and lichenification. Pigmentary changes can also be found in children. Management includes topical emmolients and topical corticosteroids. Drugs from the antihistaminic class is often used for management of pruritis.
Hence, an elementary knowledge of commonly occurring dermal diseases in pediatric age group can help parents to identify the abnormal changes at the earliest and a visit to a skin specialist, Dermatologist can help in early diagnosis and prompt treatment without compromising on the growth and development and other activities of the children.
Just beneath the surface of the skin crops up the infectious Cellulitis and erysipelas that are caused by variety of factors. Any area of the skin can be affected by Cellulitis and erysipelas but the leg is the most common site.
Starting point over these illnesses may be bacteria introduced to the skin through cuts or sores, ulcers, skin injuries, insect or animal bites, and surgical wounds. Some skin conditions like impetigo, eczema, fungal infections, such as athlete’s foot also increase the likelihood of a person getting erysipelas.
Swollen and shiny with red streaks above the affected area depicts the condition. Also a warm and tender to touch skin is a sign of cellulitis. In severe cases, skin can get blisters, turn purple or black.
Skin is met with Erysipela due to some medications that can weaken the immune system. These medications include certain cancer drugs and drugs usually used after organ transplants. Erysipelas can happen to anyone, but it most common among infants and adults over 60 years. Erysipelas is not communicable or genetic.
A clinical evaluation or blood test is performed to determine levels of white blood cells (WBC). The higher the level of WBC, the greater the tissue damage and bacterial infection caused. A computed tomography (CT) scan or magnetic resonance imaging (MRI) is necessary in some cases of severe deeper infection. In general, diagnose of erysipelas can be made by the symptoms and appearance of the affected area, because the symptoms tend to occur only with this specific condition.
Erysipelas is curable and there is no scarring. It is crucial taking up as early as possible treatment to halt the chance of further risk factors. Exact type of treatment will depend on what bacteria is causing the infection, but it will often contain penicillin. Alternate for people allergic to penicillin is cephalexin or erythromycin.
Other than medical aid, in order to speed up healing and prevent returining, one can keep the infected area elevated, place cooling packs on the skin, moisturize skin from getting dry and cracking and use compresses stocking after the problem has disappeared.
Infection will generally go away with a course of antibiotic medication. However, if you have a cellulitis of the leg, try n keep your foot raised higher than your hip as much possible. This helps to prevent clotting and excess swelling.
Dr. Batra is best practicing dermatologist in Delhi and is an eminent name in treating skin infections among infants and child. He is currently serving as head & director of DermaWorld Skin & Hair Clinics, New Delhi and is also consultant dermatologists at Sir Ganga Ram Hospital. Dr. Batra is a dedicated dermatologists and skin specialist with extensive experience of more than 2 decades across treatment of variety of skin related issues, and dealing with skin issues for new born babies and adults, specializing in aesthetic medicine, laser surgery and cosmetics skin treatments.
Such is the experience and depth of knowledge of Dr. Batra that he is visiting adjunct faculty at USCI, Kula Lumpur. He in the past has held important positions like, Joint Secretary and Convener, People Connect Cell at National IADVL in year 2015 and 2016 respectively. He is also founder & organizing secretary of DAAS Summit. He has been invited to various events and conventions on dermatologists as a guest speaker.
Sir is specialized in area of Vitiligo, laser treatments and is pioneer in handling his patients with utmost care and comfort, treating patients across all age groups. Dr. Batra himself supervises each surgery, so that his experience and research could be used to provide the patient desirous result, with utmost care and comfort.
Dr. Rohit Batra has an eye for detail, expert of preventive care, proper treatment plans, decision making under pressure, love children and to interact with patients, post treatment consultation and above all an honest medical practitioner, who uses gold standards technology for treatment of all skin related issues. He uses state of the art latest technologies for skin treatment which are cost effective and painless.
For more information or to book an appointment please click here.